January 30th 2025
FDA clearance of Pain Therapy in the US
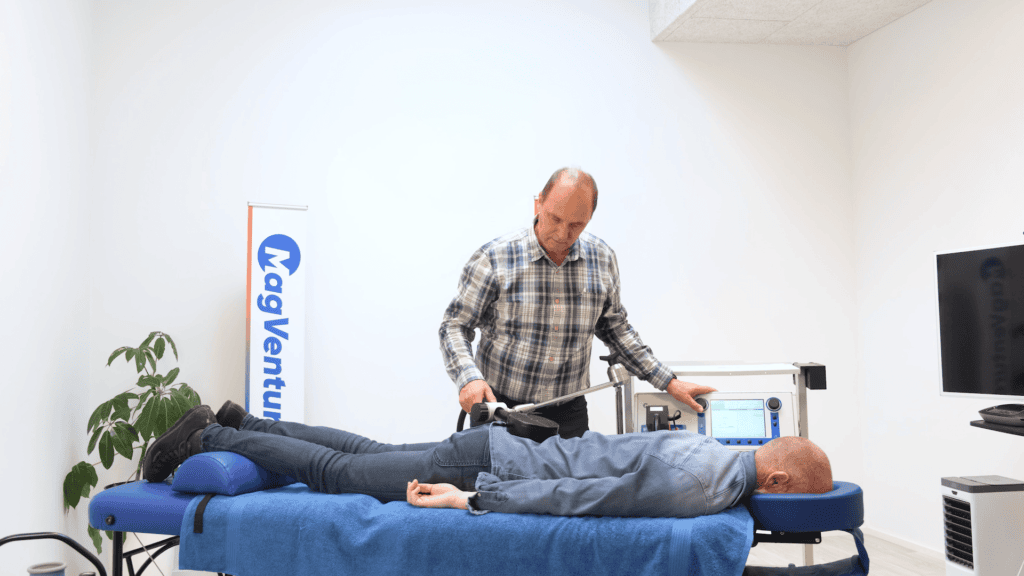
MagVenture announces FDA clearance of Pain Therapy in the US: A non-invasive approach to CHRONIC PAIN relief
Alpharetta (GA), November 30th, 2023
MagVenture, celebrates a new milestone with the launch of MagVenture Pain Therapy—an FDA-cleared solution for chronic pain relief. With over 30 years of experience, MagVenture has been at the forefront of using magnetic stimulation to enhance the lives of patients suffering from depression and other psychiatric disorders. Now, with the introduction of MagVenture Pain Therapy, we are extending its expertise to bring those solutions to chronic pain.
“Today, we take all our experience and commitment to patient care to new heights. We’re excited about the possibilities of expanding our technology to reach individuals who are living with chronic pain, offering them our perspective on pain management”, says Kerry Rome, Senior Vice President of Sales at MagVenture Inc. He expressed the company’s pride in having helped countless patients with depression using their TMS technology over the years.
MagVenture Pain Therapy employs powerful focused magnetic pulses directed near the injured nerve, providing a non-invasive, painless approach to stimulate peripheral nerves for clinically proven pain relief. Unlike traditional treatments for chronic nerve pain, MagVenture Pain Therapy offers a unique neuromodulation technique.
What sets MagVenture Pain Therapy apart is its versatility and ease of use. Patients can experience relief with sessions lasting just 13 minutes, spread over a two-month period. This non-pharmacologic treatment is a significant advancement for those seeking a safe, efficient alternative to surgery or medication for chronic pain relief.
For more information about MagVenture Pain Therapy and its potential applications, please visit www.magventurepaintherapy.com.
MagVenture Pain TherapyTM FDA Indications for Use: “To stimulate peripheral nerves for relief of chronic intractable, post-traumatic and post-surgical pain for patients 18 years or older“
For more information, please contact:
Kerry Rome, Senior Vice President, MagVenture Inc. (USA) | +1 888 624 7764 | kr@magventure.com
Media inquiries:
Esben Rosenberg, Global Marketing Manager, MagVenture A/S (DK) | +45 51465592 | ers@magventure.com
